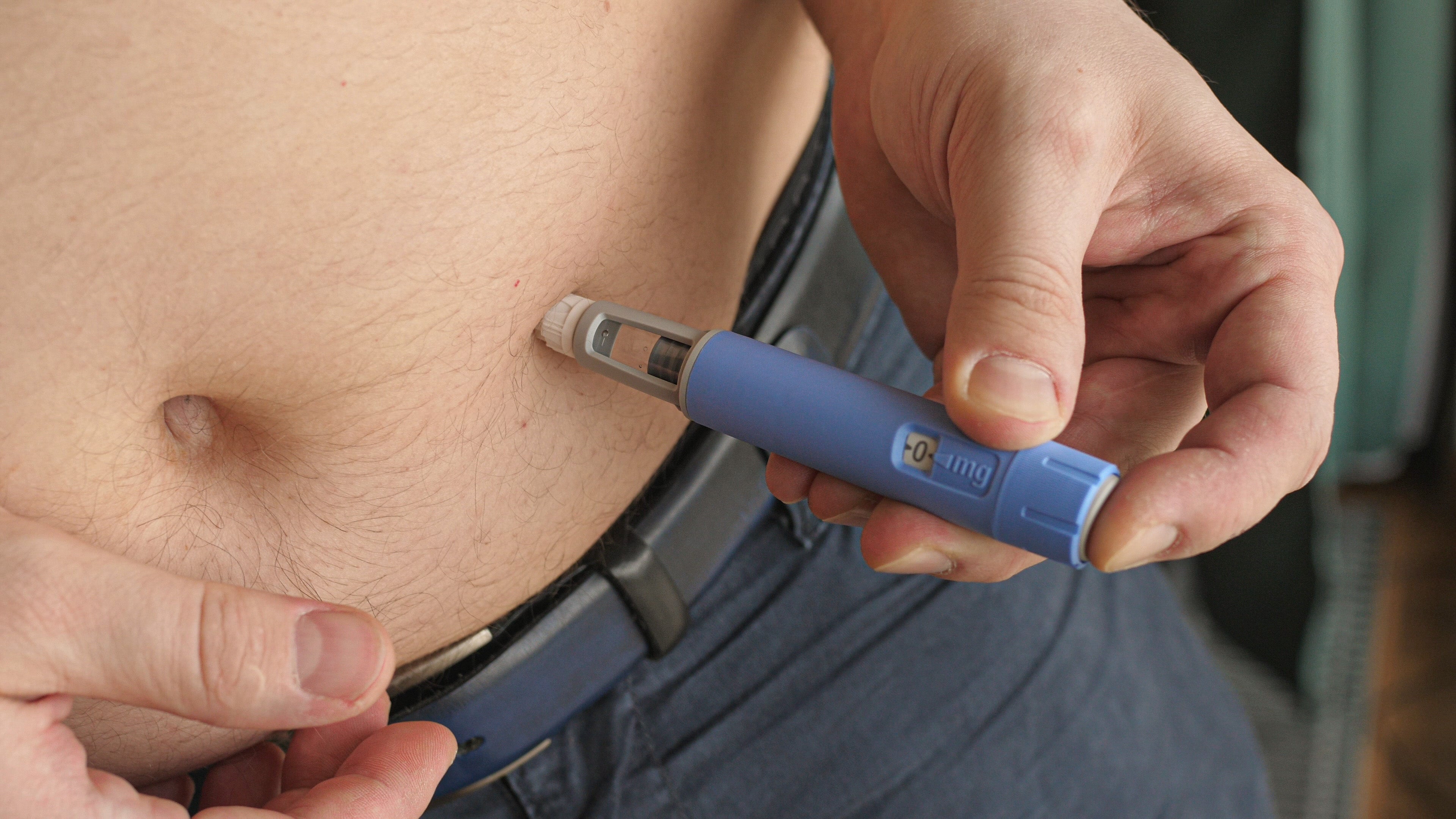
The Future Of Weight Loss Drugs: Debunking Myths And Exploring What's Next
As bariatric surgery patients, we are well aware of the crucial role weight loss plays in enhancing overall health and quality of life. In recent years, the introduction of innovative weight loss drugs, such as Ozempic, Wegovy, and Mounjaro, has brought a new level of excitement to the management of type-2 diabetes and obesity. However, despite their promise, these drugs are often subject to myths and misconceptions that are prevalent on social media.
One of the weight loss drugs available today is Mounjaro, which is FDA-approved for the treatment of type-2 diabetes and is being prescribed off-label for obesity due to the shortage of Wegovy, an FDA-approved obesity drug. Mounjaro may prove to be even more effective than Ozempic and Wegovy, as it targets multiple receptors involved in appetite, metabolism, nutrient partitioning, and lean muscle mass retention.
The future of obesity medicine is focused on the development of compounds that target multiple receptors in the body related to weight loss. For instance, CagriSema, a combination of cagrilintide and semaglutide, is a promising new drug that mimics amylin, a hormone that affects satiety. Another exciting compound is retatutride, a GLP-1/GIP/glucagon agonist, which has the potential to increase energy expenditure and calorie burning.
Additionally, ongoing studies are exploring the tolerance of higher doses of GLP-1 agonists, such as AMG-133, a GLP-1 agonist with an antibody that inhibits GIP. The order of approval for these drugs may also change, with some compounds like AMG-133 being studied for obesity first.
It's important to note that these drugs are not a new trend driven by the pharmaceutical industry, but rather the result of decades of research and development, starting with the first GLP-1 agonist approved in 2005.
Let's dispel some of the prevalent myths surrounding these drugs:
Myth 1: People should not use drugs like Ozempic and Mounjaro for weight loss alone. The truth is that obesity is a chronic disease that has been classified as such since the 1990s and increases the risk of various health issues, including type-2 diabetes, cardiovascular events, and Covid-19 complications. Seeking medical treatment, whether through bariatric surgery or FDA-approved weight loss drugs, should not be stigmatized.
Myth 2: These drugs can be taken for weight loss and then discontinued. These drugs are meant to be taken indefinitely and can only be effective with consistent use. Going on and off these drugs may result in a yo-yo effect on appetite and weight, and many patients may need to continue taking at least a low dose of these medications to manage their weight.
Myth 3: These drugs are suitable for minor weight loss. These drugs should only be prescribed by a qualified physician and are only meant for patients with a type-2 diabetes or obesity diagnosis. Taking these drugs without medical oversight can be dangerous.
Myth 4: These drugs are addictive or habit-forming. Dependence on these drugs is necessary to maintain benefits, but they are not addictive or habit-forming in the traditional sense. There is no evidence of withdrawal symptoms or cravings when discontinuing these drugs.
Myth 5: These drugs have dangerous side effects. Like all medications, there is a risk of side effects with weight loss drugs, but they are generally mild and manageable, such as nausea or diarrhea. The benefits of these drugs far outweigh the risks for many patients, especially when compared to the health risks associated with obesity and type-2 diabetes.
Myth 6: These drugs only provide short-term effects. The effects of these drugs are not limited to the short term, and patients who take these drugs consistently can expect sustained weight loss as long as they maintain healthy lifestyle choices and work with their doctor.
Myth 7: No diet or exercise changes are required for these drugs to be effective. While these drugs can help regulate appetite and insulin levels, they are not a panacea for weight loss. To achieve optimal results, patients must make healthy lifestyle choices, including a balanced diet and regular exercise.
In conclusion, the next generation of weight loss drugs holds great promise for the management of obesity and type-2 diabetes. These drugs offer a safe and effective way for patients to manage their condition, but they are not a replacement for a healthy lifestyle. It's essential to work with a qualified doctor to determine the best course of action and dispel the myths surrounding these drugs. Above all, it's important to remember that everyone deserves respect and dignity, regardless of their body size or shape.